Is your fatigue stronger than your morning coffee?
Are you losing more hair than usual?
Do you constantly feel colder — or hotter — than everyone else around you?
These subtle signs may point toward a thyroid imbalance.
Thyroid disorders are significantly more common in women because thyroid function is deeply influenced by hormonal transitions — puberty, menstrual cycles, pregnancy, postpartum recovery, and perimenopause.
If you’ve been diagnosed with a thyroid condition — or suspect something isn’t right — this expert guide will walk you through:
- Why thyroid disorders are more common in women
- How to test accurately (and avoid false results)
- Evidence-based strategies to support thyroid health
- How and when to take medications correctly
- Special precautions during pregnancy and postpartum
Let’s begin with the basics.
What Is the Thyroid Gland?
The thyroid is a small, butterfly-shaped gland located at the base of your neck. Despite its size, it regulates nearly every major system in your body.
It produces two primary hormones:
- T4 (thyroxine)
- T3 (triiodothyronine) — the active form
These hormones:
- Regulate metabolism and energy production
- Influence heart rate
- Support mood and cognition
- Affect hair and skin health
- Regulate menstrual cycles and fertility
- Support pregnancy
- Help maintain bone health through calcitonin regulation
When thyroid hormone levels are balanced, the state is called euthyroid.
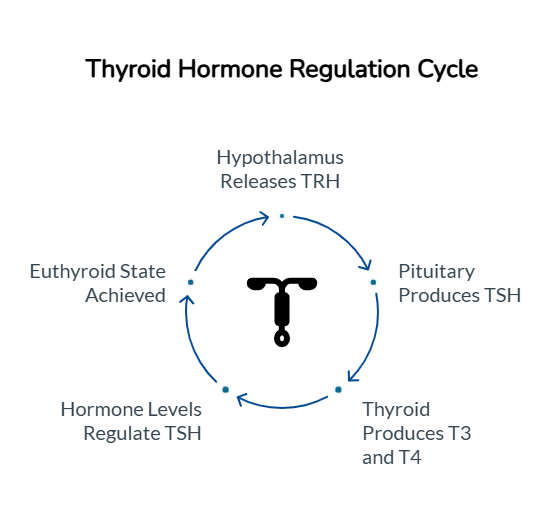
How the Thyroid Works (The Brain–Thyroid Axis)
The thyroid does not work alone.
- The hypothalamus releases TRH (thyrotropin-releasing hormone).
- TRH signals the pituitary gland to release TSH (thyroid-stimulating hormone).
- TSH tells the thyroid how much T3 and T4 to produce.
If T3 and T4 are low → TSH increases.
If T3 and T4 are high → TSH decreases.
Any disruption in this feedback loop can lead to thyroid dysfunction.
Common Thyroid Disorders in Women
1. Hypothyroidism (Underactive Thyroid)
Thyroid produces too little hormone.
Symptoms:
- Fatigue
- Weight gain
- Cold intolerance
- Constipation
- Hair thinning
- Heavy or irregular periods
Most common cause: Hashimoto’s disease (autoimmune)
2. Hyperthyroidism (Overactive Thyroid)
Thyroid produces excess hormones.
Symptoms:
- Unexplained weight loss
- Heat intolerance
- Palpitations
- Anxiety
- Insomnia
- Missed periods
Most common cause: Graves’ disease (autoimmune)
3. Postpartum Thyroiditis
Occurs within the first year after childbirth.
- Early phase: hyperthyroid symptoms
- Later phase: hypothyroid symptoms
- Often mistaken for “new mom stress”
4. Goiter
Enlargement of the thyroid gland.
- Visible neck swelling
- Difficulty swallowing
- Coughing or pressure sensation
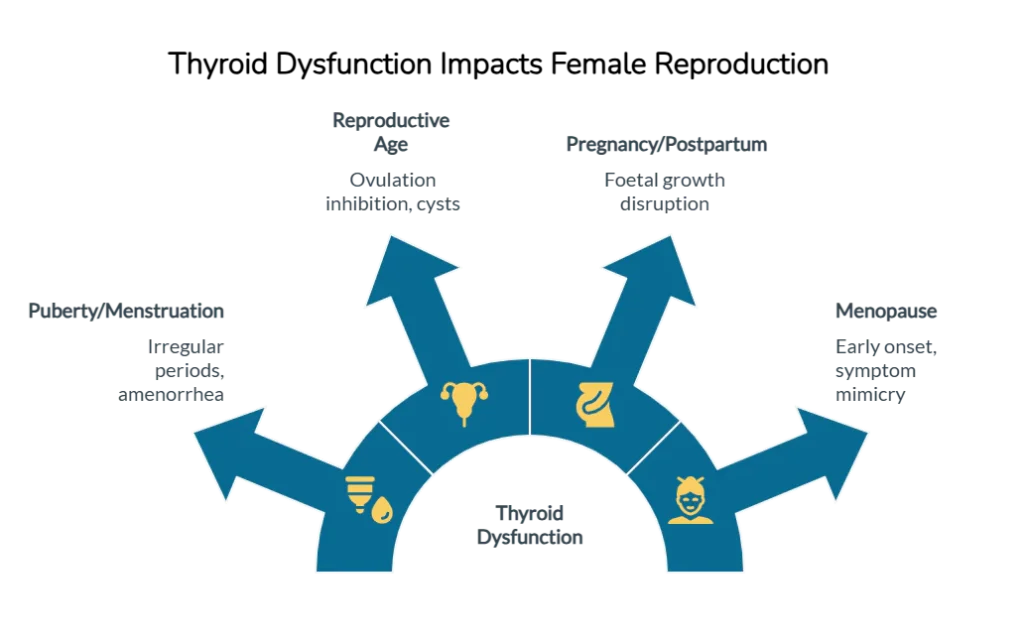
Why Are Thyroid Disorders More Common in Women?
Approximately 1 in 8 women will develop a thyroid disorder in her lifetime.
Here’s why:
1. Lifelong Hormonal Shifts
Women experience multiple endocrine transitions:
- Puberty
- Monthly menstrual cycles
- Pregnancy
- Postpartum immune rebound
- Perimenopause
During pregnancy:
- Estrogen increases thyroxine-binding globulin (TBG)
- Total thyroid hormone demand increases
After delivery:
- The immune system rebounds
- Autoimmune thyroiditis risk increases (5–10%)
2. Stronger Immune Reactivity (X-Chromosome Influence)
Women have stronger immune responses — beneficial for infection defense but higher risk for autoimmunity.
Thyroid peroxidase (TPO) and thyroglobulin (Tg) antibodies are nearly twice as common in women.
Risk increases with age.
Who Is at Higher Risk?
- Women 40–50 years
- Postpartum (within 12 months)
- Perimenopause
- Individuals over 60
- Family history of thyroid or autoimmune disease
- History of neck radiation
- Prior thyroid surgery
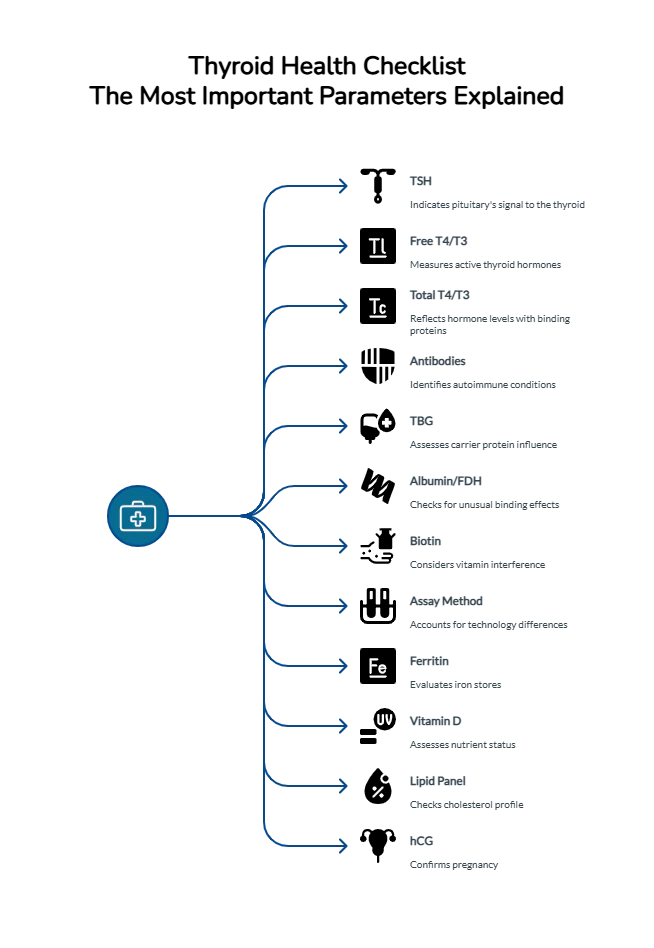
How to Diagnose Thyroid Disorders Correctly
Thyroid diagnosis is not symptom-based alone.
Essential Blood Tests
TSH
- High → Hypothyroidism
- Low → Hyperthyroidism
Free T4 and Free T3
- Measure circulating active hormones
Anti-TPO & Anti-TG Antibodies
- Detect autoimmune thyroid disease
Imaging (When Needed)
- Thyroid ultrasound (nodules, size)
- Thyroid scan
- Radioactive iodine uptake test
How to Avoid False Test Results
- Stop high-dose biotin 48–72 hours before testing
- Test at the same time of day consistently
- Do not take thyroid medication before blood draw
- Follow fasting instructions if advised
Consistency prevents misinterpretation.
Medications Your Doctor May Prescribe
For Hypothyroidism
- Levothyroxine (LT4)
For Hyperthyroidism
- Methimazole
- Propylthiouracil
Symptom Control
- Beta blockers (for palpitations)
Never self-prescribe supplements marketed as “thyroid boosters.”
Expert Strategies to Support Thyroid Health
Testing shows where you are.
Treatment restores balance.
Lifestyle helps maintain it.
1. Build a Balanced Diet First
Follow core nutrition principles:
- 5 portions of fruits and vegetables daily
- Iodized salt (in moderation)
- Dairy or fortified alternatives (iodine + selenium)
- Whole grains
- Lean protein (beans, fish, eggs, meat)
- Unsaturated fats
- Limit processed sugar
Cruciferous vegetables and soy are safe in normal cooked amounts.
2. Key Nutrients for Thyroid Support
Iodine
Essential but excess can worsen autoimmune disease.
Selenium (200 mcg/day in some studies)
May reduce antibodies in select cases.
Vitamin D
Commonly deficient in autoimmune thyroid disease.
Zinc
Supports TRH production.
Omega-3 fatty acids
Reduce systemic inflammation.
Vitamin A
Supports thyroid–pituitary signaling (avoid unsupervised supplementation).
Always test before supplementing.
3. Take Medication Correctly
- Take levothyroxine on an empty stomach
- Same time daily
- Wait 3 hours before iron or calcium
- Report symptoms of over/under-treatment
- Vitamin C may improve absorption (doctor-guided)
Consistency matters more than dose perfection.
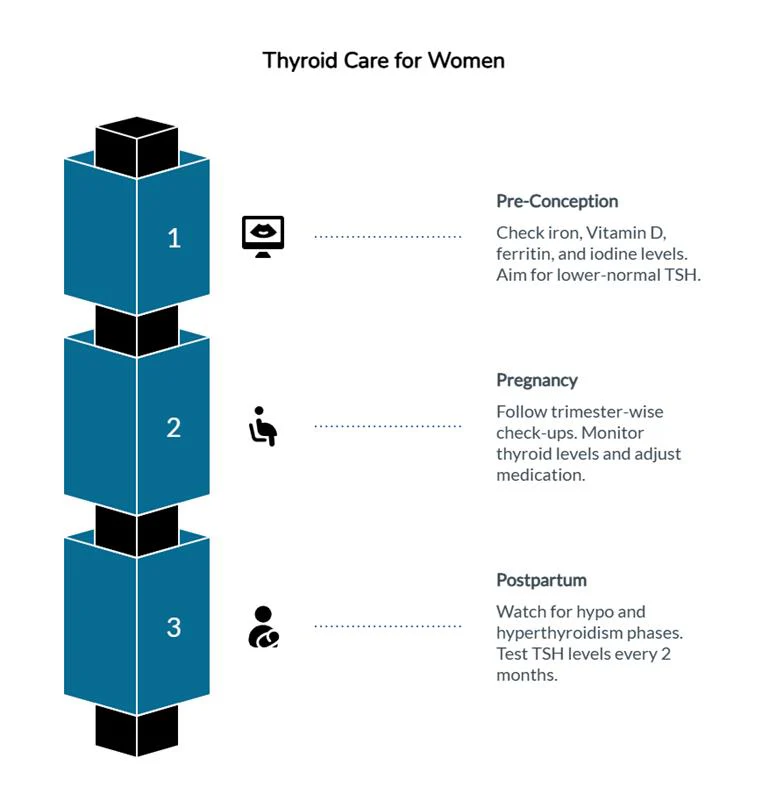
4. Pregnancy & Thyroid: What Women Must Know
Trying to Conceive
- Target TSH: 1–2.5
- Correct iron and vitamin D deficiencies
- Discuss possible LT4 dose adjustment
During Pregnancy
- Frequent monitoring, especially first trimester
- Dose adjustments common
Postpartum (0–12 months)
Watch for:
- Racing heart
- Anxiety
- Fatigue
- Mood shifts
Advocate for testing if symptoms appear.
5. Lifestyle Foundations
Exercise
At least 150 minutes moderate activity weekly.
Include:
- Cardio
- Strength training
- Gentle yoga (shown to improve quality of life in thyroid patients)
Sleep
7–9 hours nightly.
Poor sleep increases thyroid vulnerability.
Stress Management
Chronic stress elevates cortisol, which may blunt thyroid signaling.
Strategies:
- Breathwork
- Journaling
- Digital detox before bed
- Structured relaxation time
Final Thoughts
Thyroid imbalance doesn’t just affect your labs — it affects your energy, fertility, mood, metabolism, and identity as a woman.
But here’s the empowering truth:
- Early symptom recognition
- Accurate testing
- Precise medication
- Smart nutrition
- Consistent lifestyle habits
Together, they restore balance.
If something feels off — don’t ignore it.
Test smart. Treat right. Stay consistent.

Leave a Reply